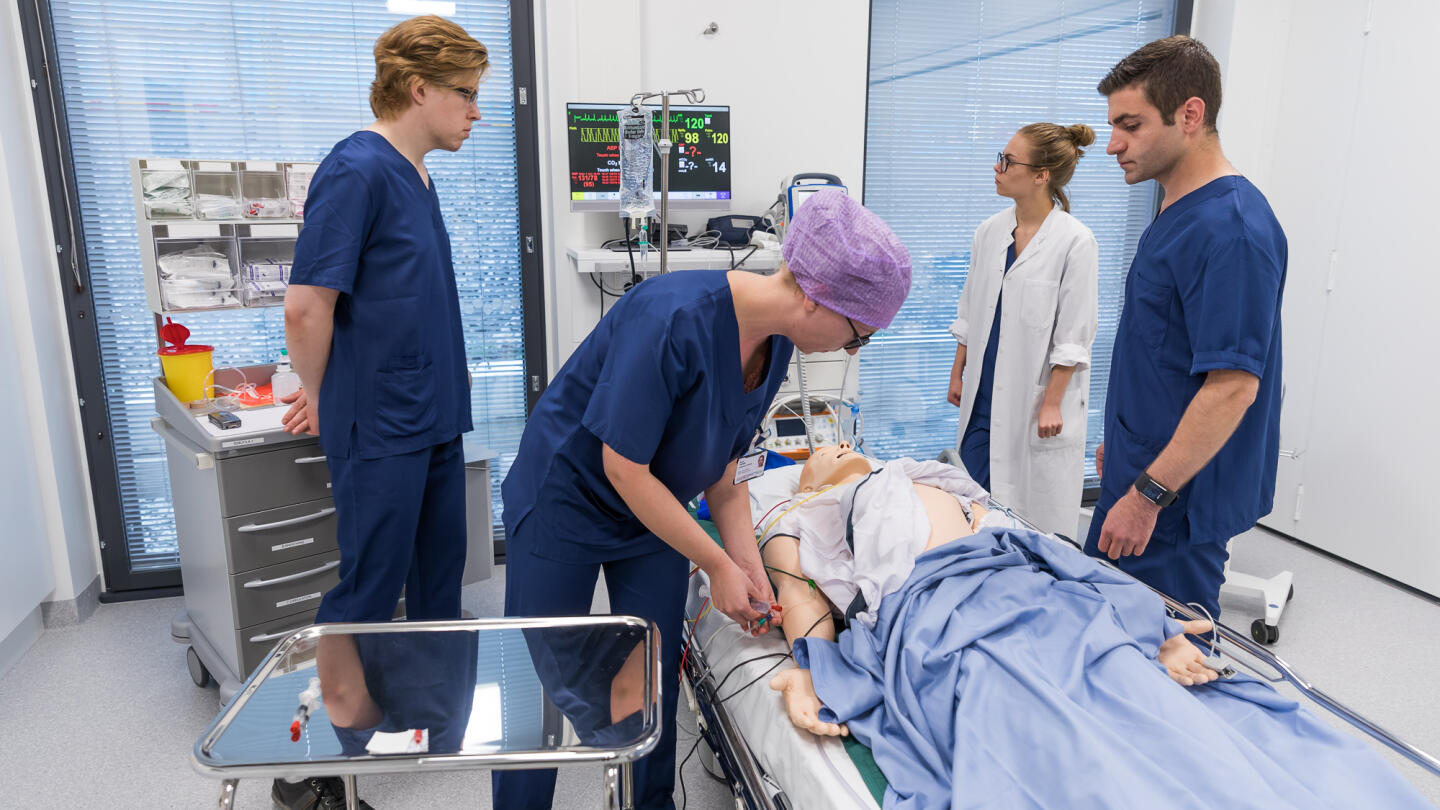
Finland’s high quality healthcare is ensured by training qualified experts in medicine and nursing sciences. In the new clinical skills teaching facilities of the University of Turku, future doctors and nurses can simulate working in multiprofessional groups, using various practical skills. While the patient in the room happens to be a dummy, the simulation creates real learning experiences.
A man complaining of accelerated heartbeat has a arrived at a hospital emergency room. Simo Virtanen, born in 1958, was jogging four hours ago when his heart started to beat exceptionally quick. He stopped running, went back home and lied down. As the unpleasant beating continued, he took a taxi to the hospital.
Two emergency care nurses enter the room. In the bright white lights of the hospital, it's difficult to see them at first. The men greet the patient and start asking questions about his condition.
– Let's start with some basic readings, we’ll just attach these electrodes on you. The doctor will see you shortly, the nurse says.
Soon, the on-duty internal medicine specialist arrives. The nurses give her a short description of the case. The doctor asks the patient about the situation he was in when the palpitations started, his medical records and any possible risk factors.
– Have you done anything out of the ordinary recently? Did you drink last night? Do any heart diseases run in your family? Do you smoke?
As the patient's pulse is over 130, the doctor prescribes two milligrams of beta blocker Seloken to slow down the heartbeat and make the patient more comfortable.
– A recent atrial fibrillation, the rhythm can be converted electrically. It’s a small jolt. You will get some anaesthetic, we’ll give you a little shock, and see if your heart rate comes back to normal, the doctor calmly explains to the patient.
While the nurses and the doctor are interviewing the patient and conducting necessary measurements, they are addressing him respectfully and constantly checking that his condition is as good as can be, or at least that it's not taking a turn for the worse.
The human interaction with the patient doesn't always feel natural, as the patient laying on the hospital bed is not a living breathing human, but a dummy.
Briefing
The patient's real name isn't Simo Virtanen. He is SimMan 3G, a clinical simulation mannequin. And instead of an actual hospital emergency room, the students have gathered in SimuCenter, a recently finished simulation facility on the second floor of the brand new Medisiina D building.
SimuCenter, like the entire Medisiina D building, is shared between the University of Turku, the Hospital District of Southwest Finland, and the Turku University of Applied Sciences.
– This makes conducting multiprofessional simulations possible. Once the entire clinical pathway is embedded in the simulation, students get a better picture of a real hospital environment, says SimuCenter's coordinating Teaching Nurse Minna-Kaarina Wuorela.
A multiprofessional simulation training session is beginning in Medisiina D. The people participating in the electric cardioversion of acute atrial fibrillation simulation are University of Turku’s sixth year medical students Amanda Seppälä and Sanna Tähkäpää, as well as emergency care students Santeri Koivumaa and Rizgar Yousif from Turku University of Applied Sciences.
Before the exercise begins, Wuorela and Clinical Lecturer, Staff Anaesthesiologist Matias Rantanen go through a pre-briefing of the simulation with the students. The students are shown around the simulation room. Rantanen lists the simulation's learning goals.
– You need to perceive when it's necessary to do a cardioversion and understand its practicalities, especially the operation of a defibrillator. As electrical cardioversion requires anaesthesia, the student needs to understand how a short-term anaesthesia is done safely, meaning what to do before anaesthetising the patient and how to secure vital functions during the anaesthesia. If necessary, the emergency nurses need to be able to support doctors and perform practical tasks.
Wuorela says that the simulation is an extraordinary teaching tool, as it allows for the practice of various skills simultaneously.
– Technical and non-technical, interaction, teamwork, leadership, situational awareness and patient safety. The non-technical goals of the exercise includes the efficient flow of information within the team and that the entire team participates in observing changes in the patient's condition.
In the simulation, the students work independently but under supervision. When the students talk to the synthetic patient, Rantanen’s voice emanates from a speaker installed in the dummy's mouth.
– What's an atrial fibrillation then? the teacher in the role of the patient asks the doctor.
Rantanen and Wuorela are sitting in the control room, separated from the simulation by a one-way mirror. The room is equipped with computers the teachers can use to control the simulation dummy's functions. For instance, the dummy can be set to suffer convulsions and its respiratory frequency and pupil size can be adjusted. With the microphones in the control room, the supervisors can communicate with the students in the role of the patient and as directors via a speaker on the ceiling.
Simulation
Once Seppälä, in her role as internal medicine specialist, has done the necessary procedures, she calls upon acting anaesthesiologist Seppälä to anaesthetise the patient prior to electrical cardioversion.
– The patient has been feeling well, but suffered a sudden atrial fibrillation while jogging. As the patient has no risk factors, the A-fib can be converted without preceding anticoagulant treatment, explains Seppälä to Tähkäpää.
After the patient is anaesthetised, all four students start buzzing around him. Koivumaa is pulling beta blocker medication into a syringe and Yousif is setting defibrillator electrodes on the patient's chest. Seppälä starts up the defibrillator while Tähkäpää is giving the patient oxygen by hand.
– Remember that you have to stop giving the oxygen once the defib hits, says Seppälä.
Soon the room is filled by the defibrillator’s beeping, which quickens to a continuous warning tone.
– Clear, warns Seppälä.
– Clear! exclaim the three others.
With the push of a button, the electrocardiogram readings begin normalising.
– The heart rate may be dropping a bit too low. Prepare half a milligram of Atropine, Tähkäpää says to Koivumaa.
– Found the sinus rhythm. Let’s try lifting the patient’s legs a bit, says Seppälä to Yousif, who fetches a pillow to support the patient’s legs.
– The heart rate is rising again. Let's see whether Atropine is required.
– Should I inject? There’s still time. Heart rate 61, says Koivumaa.
There's a moment of uncertainty, before the anaesthesiologist on call, Tähkäpää, takes control of the situation.
– If the patient jogs a lot, this could be his normal heart rate. Let’s keep an eye on this.
A moment later, the situation has remained stable and the medication is not required.
– Thank you all, this concludes the simulation, sounds Rantanen's voice from the ceiling speaker.
Debriefing
The simulation is over and the students relax.
– Should we begin by unravelling all the gear or the things we did? asks Seppälä, laughing.
A debriefing always follows the simulation. The students and teachers go through a descriptive, analytical feedback discussion that sums up the exercise.
– It’s also the most educational phase in the simulation, says Wuorela.
The group of students and teachers moves into the smaller room on the other side of the hallway. It features a giant screen that shows video footage of the simulation room. Clinical Lecturer Rantanen leads the discussion and asks the students to talk about their actions during the simulation.
Rantanen and Wuorela, who both have gone through simulator teacher training, explain that their training focused especially on debriefing and guidance as teaching tools, instead of the practicalities of the technology. The debriefing requires a teacher to first and foremost possess pedagogical skills and practical expertise.
Once the students have reflected on their actions, they receive feedback from the Clinical Lecturer and fellow students. Whereas the simulation itself is over in fifteen minutes, the debriefing can take close to an hour.
The atmosphere is positive and calm, and the students have a hard time keeping a straight face. After the thrilling exercise, the students are in a cheerful mood.
– We need to be careful when planning the simulations, so that the students don’t experience them like a traumatic school exam, says Rantanen once the students have left the room.
Despite the fact that the simulation provides a safe environment for students to practice challenging patient encounters, the situation can be nerve-racking. While the students have finished packing up their gear and are leaving the simulation facility, medicine student Sanna Tähkäpää has time to share her thoughts.
– The simulations are thrilling and genuinely educational, she says.
Text: Heikki Kettunen
Photos: Hanna Oksanen
Translation: Mikko Suhonen